Varicose Veins
Learn about the symptoms, causes, treatments, & prevention of varicose veins. Call Mackay Vein for a consultation today at 727-527-2888.
Dr. Mackay is the leading board certified Vascular Surgeon with offices in St. Pete, Palm Harbor, & Largo, Florida.
What are Varicose Veins?
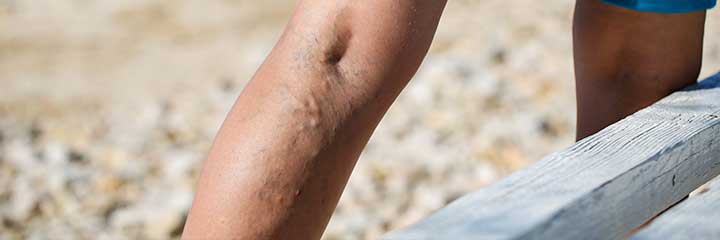
Veins are found through the body and move blood from the body back toward the heart. When veins no longer work properly, they are unable to push blood back toward the heart, which causes the veins to fill with blood and swell. They then appear on the skin surface as twisted and tortuous veins.
How are varicose veins treated?
There are several different treatment options available to treat varicose veins. Multiple factors may play into which procedure may be the right procedure to treat your varicose veins.
Sclerotherapy: This is an office-based procedure that uses a small incision into the vein in order to inject a chemical called a sclerosant into the veins. The sclerosant causes irritation to the vein wall that will cause the vein to scar down completely, preventing further blood flow. Over time, the body removes the nonfunctional vein.
Endovascular Laser Therapy (EVLT): This is an office-based procedure that uses a small incision to insert a laser device into the veins. The laser uses heat to destroy the inside of the vein, causing eventual scarring and prevention of blood flow. The body eventually removes the scarred vein.
Vein stripping: This is a surgical procedure in which the varicose veins are completely removed from the body. It is used less commonly now, due to the success and minimally invasive techniques of sclerotherapy and EVLT.
Varicose Vein Treatment Before & After Photos
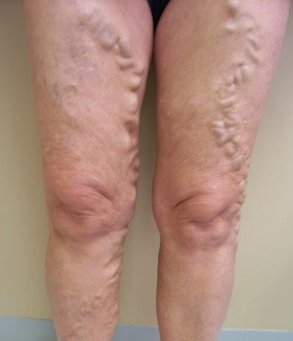
Before (case 1)
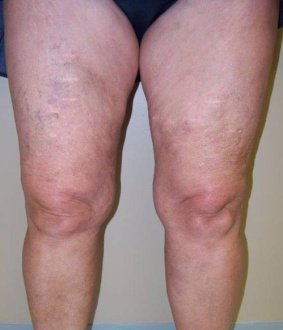
After (case 1)

Patrice K. - Google Review
I've been going to Dr Mackay for vericose and spider vein issues for years and have gotten to witness not just the latest technology available, but that technology being utilized by one of the highest rated vascular surgeons in the country. He is incredibly skilled, and he is a kind and genuinely wonderful person . Every one of his staff is also the highest caliber, and treat patients with respect. I drive 45 minutes to get to the office, and would drive twice that. Dr. Mackay is the best. Wish I could rate him more than 5 stars!
What causes varicose veins?
Veins are thin, floppy tubes that can easily collapse. They are responsible for moving blood from the body back toward the heart, with the use of one-way valves that are found within the veins and the contraction of the body muscles. The one-way valves are interspersed through the veins and prevent blood from flowing backwards, while the muscles contract and squeeze the veins to push blood through. If the valves weaken, they are unable to close fully, and then blood accumulates in the veins causing swollen varicose veins.
Varicose veins are seen most commonly in the feet, calves, and thighs, as the blood in the legs has to move against gravity to move towards the heart. This causes more problems with failing valves and accumulation of blood in the veins.
Are there risk factors for varicose veins?
There are certain reasons that can increase the risk for developing varicose veins.
- Age: The older someone is the more likely their veins will be susceptible to failing valves and varicose veins. Veins begin to lose elasticity with age, which makes them more susceptible to pressure changes and failing valves.
- Sex: Females are at a higher risk to develop varicose veins, as hormonal changes in the cycle, puberty, pregnancy, use of hormonal contraceptives, and menopause may all cause varicose veins.
- Family history: There is likely a genetic component for weak veins, malfunctioning valves, or both. Around half of people with varicose veins have a family member that also has varicose veins.
- Weight: Increased body weight from being overweight or obese places pressure on the veins, which can cause them to weaken and the valves to malfunction.
- Activity: Staying in static positions, either sitting or standing, most of the time, prevents the muscles from contracting and pushing the blood out of the veins, which over time can cause varicose veins.
- Pregnancy: Due to hormonal changes, increasing weight, and pressure on the veins in the abdomen from the growing baby, pregnancy is a common reason women develop varicose veins.
What are the symptoms of varicose veins?
There are several different symptoms of varicose veins, but there are variations in the severity of symptoms, as some people do not have any symptoms at all. The symptoms are related to the excess pressure within the varicose veins and the movement of fluid from the vein to the surrounding tissues due to the vein swelling.
Leg swelling, particularly at the end of the day
Bulging veins
Cramping of the legs
Heaviness in the legs
Tired legs
Pigmentation changes of the legs
Redness of the skin
Dry, flaking skin
Hardened veins on the skin surface
What are the complications of varicose veins?
Varicose veins are a benign condition and are not usually considered a dangerous condition. For those that are left untreated with worsening symptoms, there can be certain complications.
Drainage: The excess pressure in the veins leads to the fluid portion of the blood, the serum, to move out of the vein into the surrounding tissue. If the pressure in the tissue increases, the body will try to push out the excess fluid, through the skin.
Poor healing: As there is excess fluid in the tissues, this prevents adequate nutrients in the blood from reaching the skin appropriately and this can lead to poor healing wounds and long standing ulcers on the legs, even from small skin trauma.
Skin infections: With ulcers and wounds that are open, as well as drainage from the skin, this allows the bacteria that naturally occurs on our skin to invade the skin and cause infections, such as cellulitis.
Bleeding: With engorged veins sitting just below the skin surface, trauma to the leg can cause a large amount of bleeding.
Superficial thrombophlebitis: This is a condition in which a clot forms within the smaller, superficial veins in the legs due to the pooling blood from poor circulation. This is usually felt as a cord in the vein with tenderness and surrounding redness.
Deep vein thrombosis (DVT): This is the most dangerous complication of varicose veins. DVTs are a clot within the deep veins in the leg that forms due to blood that accumulates and does not circulate. DVTs are dangerous, as this type of clot can break away from the vein and travel to the lungs, causing a pulmonary embolism, which can be deadly.
How do you prevent varicose veins?
The best way to prevent varicose veins is to try to reduce your risk factors, if possible and try to add specific things into your routine that may lessen the likelihood or even treat mild symptoms of varicose veins.
Weight loss: As being obese or overweight increases the pressure on the venous system, losing weight can help to reduce the pressure in the veins. For those without varicose veins, controlling weight is a good way to prevent varicose veins.
Changing position: If you find yourself having to sit or stand constantly at work, make a habit to walk or perform ankle pumps at your desk every hour to try and contract the muscles to move the blood from the legs.
Exercise: Performing low impact exercise, such as walking, swimming, or biking, at least 30 minutes every day can help to prevent or treat varicose veins by activating the muscles to squeeze the blood out of the legs.
Compression stockings: Wearing compression stockings that can either be purchased over the counter or with a prescription, place pressure on the muscles and legs, to facilitate movement of blood, reducing pressure in the veins.
What is the Recovery after Varicose Vein Treament
Recovery after treatment is typically minimal, but is dependent upon which procedure was performed. Always follow the instructions of your Vascular Surgeon after having a procedure.
EVLT and Sclerotherapy: As both of these procedures are performed in the office and are similar in nature, the recovery is also similar. The incision is small which only requires a small bandage for 1-2 days. Compression stockings are required for the first 2 weeks, but can also depend on the amount of veins that were treated. Walking is encouraged right away to help with blood flow and healing. Other things to consider for recovery is avoidance of swimming, bathing, and sun exposure for the first 2 weeks to prevent infection and discoloration of the skin.
Vein stripping: This procedure is performed in an operating room setting and therefore the incision is larger, requiring thicker bandages that stay in place for several days to 1 week. Due to the more invasive nature of this procedure, it takes about 2-4 weeks for recovery time with the use of compression stockings and daily walking to reduce swelling, improve blood flow, and prevent a blood clot within the veins.
Varicose Vein Post-Treatment Instructions
Download Dr. Mackay's varicose vein post-treatment instructions, click here.
When will I see results after treatment?
Results can vary based on the areas treated, severity of veins prior to treatment, and the type of treatment used.
EVLT and Sclerotherapy results: One week after treatment, there may be a noticeable difference in veins, but full effect may take several weeks to months. For those with severe or numerous veins, it may take more than a single session of these types of treatments, which will cause a delay in results.
Vein stripping results: The results are almost immediate after vein stripping, as the problematic vein is completely removed from the body, although post surgical swelling and bruising may hide the actual results until they resolve.
Why Choose Dr. Mackay for Your Varicose Veins
Dr. Mackay is a Board Certified Vascular Surgeon with the clinical expertise to treat your varicose veins. His office has state of the art equipment used to treat your varicose veins and vein problems.