Spider Veins
Learn about the symptoms, causes, treatments, & prevention of spider veins. Call Dr. Mackay for a consultation today at 727-527-2888.
Dr. Mackay is the leading board certified Vascular Surgeon Pinellas County.
What are Spider Veins?
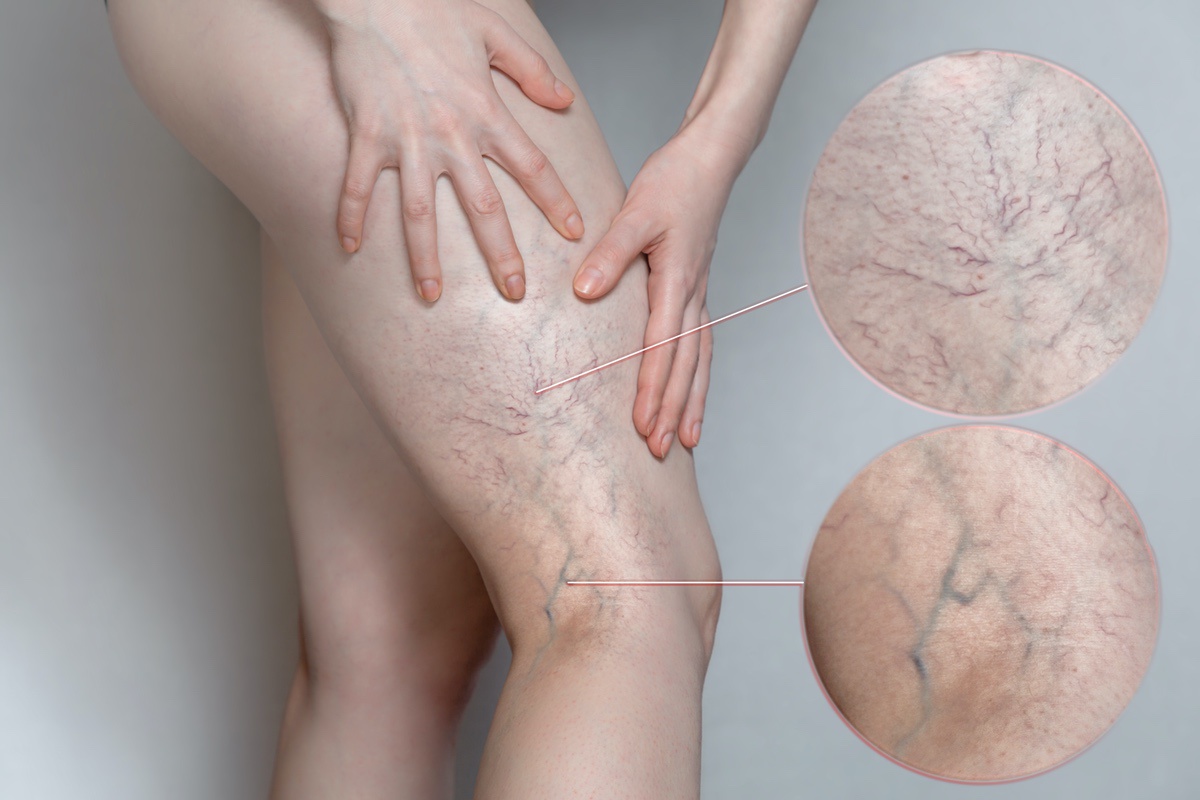
Spider veins are the small, spiculated red to blue to violet discolorations located just below the skin surface. They can be found anywhere on the body, but tend to appear most commonly on the face and the legs and are usually a source of embarrassment for many, due to their appearance.
Click a link below to go directly to that section.
- What are spider veins?
- What causes spider veins?
- Are there risk factors for spider veins?
- Symptoms of spider veins
- How to prevent spider veins
- How are spider veins treated
- What is the recovery from spider veins treament
- When will you see results after spider veins treatment
- How to choose a spider vein doctor
How are spider veins treated?
If the appearance of your spider veins has caused you to avoid wearing shorts, dresses, or bathing suits, there are procedures that can minimize and remove the spider veins. The procedure that is most recommended for the treatment of spider veins is sclerotherapy.
Sclerotherapy uses a chemical substance, a sclerosant, that is injected into the spider vein. The sclerosant damages the inside of the vein, causing the vein to scar down on itself, and it is eventually reabsorbed by the body. Sclerotherapy can be performed in several ways.
Conventional Sclerotherapy: The sclerosant used is a liquid solution.
Foam Sclerotherapy: The sclerosant is foam based which coats the veins better and can be seen on ultrasound.
Ultrasound-Guided Sclerotherapy: An ultrasound is used to identify the spider veins and is also used to administer the sclerosant to ensure the appropriate veins are treated.
Spider Vein Treatment Before & After Photos
Before (case 1)

After (case 1)

Before (case 2)

After (case 2)

Patrice K. - Google Review
I've been going to Dr Mackay for vericose and spider vein issues for years and have gotten to witness not just the latest technology available, but that technology being utilized by one of the highest rated vascular surgeons in the country. He is incredibly skilled, and he is a kind and genuinely wonderful person . Every one of his staff is also the highest caliber, and treat patients with respect. I drive 45 minutes to get to the office, and would drive twice that. Dr. Mackay is the best. Wish I could rate him more than 5 stars!
What causes spider veins?
Spider veins are similar to varicose veins, but they occur in the smaller and more superficial veins in the body. Veins are responsible for moving blood from the body back toward the heart. They are all different sizes, but have the same structure, which is a floppy tube that contains valves with flaps to move the blood in the appropriate direction.
If the valve no longer works, blood is able to build up in the vein, increasing the pressure, thus causing spider veins. Since spider veins are failures of the smaller veins close to the skin, they appear as spiculated discoloration directly on the skin surface.
Even though spider veins form due to the same reason that varicose veins form, spider veins do not cause varicose veins. It is common for spider veins to be a precursor for someone to develop varicose veins, as the presence of varicose veins usually signifies worsening of venous disease.
Are there risk factors for spider veins?
There are some risk factors that increase the chances of developing spider veins. Having these risk factors does not mean that someone will develop spider veins, but this increases the chance. Just like not having these risk factors does not mean that someone will not develop spider veins.
Family History: If other members of your family, such as your parents or siblings, have spider veins, you are more likely to develop spider veins as well.
Obesity: Carrying extra weight and being obese increases the pressure in the veins in the legs due to pressure on the veins in the abdomen, pelvis, and legs.
Stationary positions: Those people that work in jobs where they are sitting or standing for long periods of time may develop spider veins as this leads to an increased pressure in the veins in the legs.
Age: The older someone is the higher chance there is to develop spider veins, as the elasticity of the veins decline, making the valves not work as well.
Being female: The female sex is much more likely to develop varicose veins due to fluctuations in the hormones during the menstrual cycle, menopause, and pregnancy. With pregnancy, the growing fetus also places pressure on the veins in the pelvis, which can increase the pressure in the veins in the legs.
What are the symptoms of spider veins?
Spider veins are typically not painful and are mainly seen as a cosmetic concern. If multiple spider veins are present, this may potentially cause swelling in the legs, tired legs, or cramping in the legs, but these symptoms are more associated with varicose veins.
How do you prevent spider veins?
There are ways to try and prevent spider veins, or at least slow the start or progression of spider veins.
Exercise: Performing low impact exercises, such as walking, swimming, or biking, at least 3-4 days per week allows the muscles to appropriately squeeze blood through the vessels. Higher impact exercises such as running or lifting heavy weights can make spider veins worse due to the excess pressure that can build up in the veins. Exercise also is a great way to lose weight to reduce pressure on the veins, or maintain a healthy weight to prevent this pressure from developing in the veins.
Leg elevation: Elevating your legs at the end of the day helps to facilitate blood flow toward the heart to move the blood out of the veins in the legs.
Change position: If you sit or stand for long periods at work, attempt to move more throughout the day. Try to step away at least twice an hour to walk to improve circulation in the legs or perform foot pumps or calf raises to help squeeze the blood out of the legs with the contraction of the muscles.
What is the Recovery after Spider Veins
Recovery is typically minimal, as sclerotherapy is performed in the office with a small incision, covered by a band-aid. Pain is usually minimal with the use of over the counter pain medication being appropriate to treat pain. There are certain post-operative instructions after the procedure for optimal recovery.
Exercise: Walking daily for the first 1-2 weeks after the procedure increases the blood flow and healing. Speed and duration of walking slowly increases as tolerated. High impact exercises such as weight lifting and running should be avoided.
Compression stockings: Compression stockings help to reduce swelling and improve circulation, which should be worn most of the time for the first 1-2 weeks after the procedure.
Spider Vein Post-Treatment Instructions
Download Dr. Mackay's spider vein post-treatment instructions, click here.
When will I see results after treatment?
Results take several weeks to be evident and are largely variable on how many spider veins are present and how many sclerotherapy sessions are needed. Based on the way the procedure is performed, it takes the body time to react to the scarred vein and begin resorption, therefore it can take weeks to notice a difference in the spider veins.
The majority of people see full results after 4 treatment sessions, which are performed about 6 weeks apart. After all sessions have been completed, the vein has been completely removed by the body and will no longer be visible.
Why Choose Dr. Mackay for Your Spider Veins
Dr. Mackay is a board certified vascular surgeon that specializes in vascular diseases and treatments. His office consists of state of the art equipment for the appropriate diagnosis and treatment of vascular disease for optimal results.
The consultation consists of a detailed history and examination to discuss your vascular diseases, treatment options, and recommendations for your vascular disease.